Breathing
Mobile Platform.
First app that tracks mouth breathing
You sleep 8 hours. You wake up exhausted. The problem isn't how long you sleep, it might be how you breathe.
Launching in





The silent epidemic.
Mouth breathing during sleep is detrimental to airflow compared to nasal breathing. 1
of adults report night-time nasal congestion. 2
i
From a population-based sample of 4,916 adults aged 30–60.
greater airway resistance when mouth breathing. 1
i
Nose blocked vs mouth blocked during sleep resulted in apnea events increasing from 1.5 to 43 per hour — over 300 apneas per night.
don't know they stop breathing during sleep. 3
i
An estimated 936 million people suffer from sleep apnea — most undiagnosed. Where high loop gain contributes, we can help.
more likely to stop breathing when the nose is congested. 4
"Most people have no idea their breathing might be working against them every single night."
Are you a mouth breather?
Answer 4 quick questions to find out.
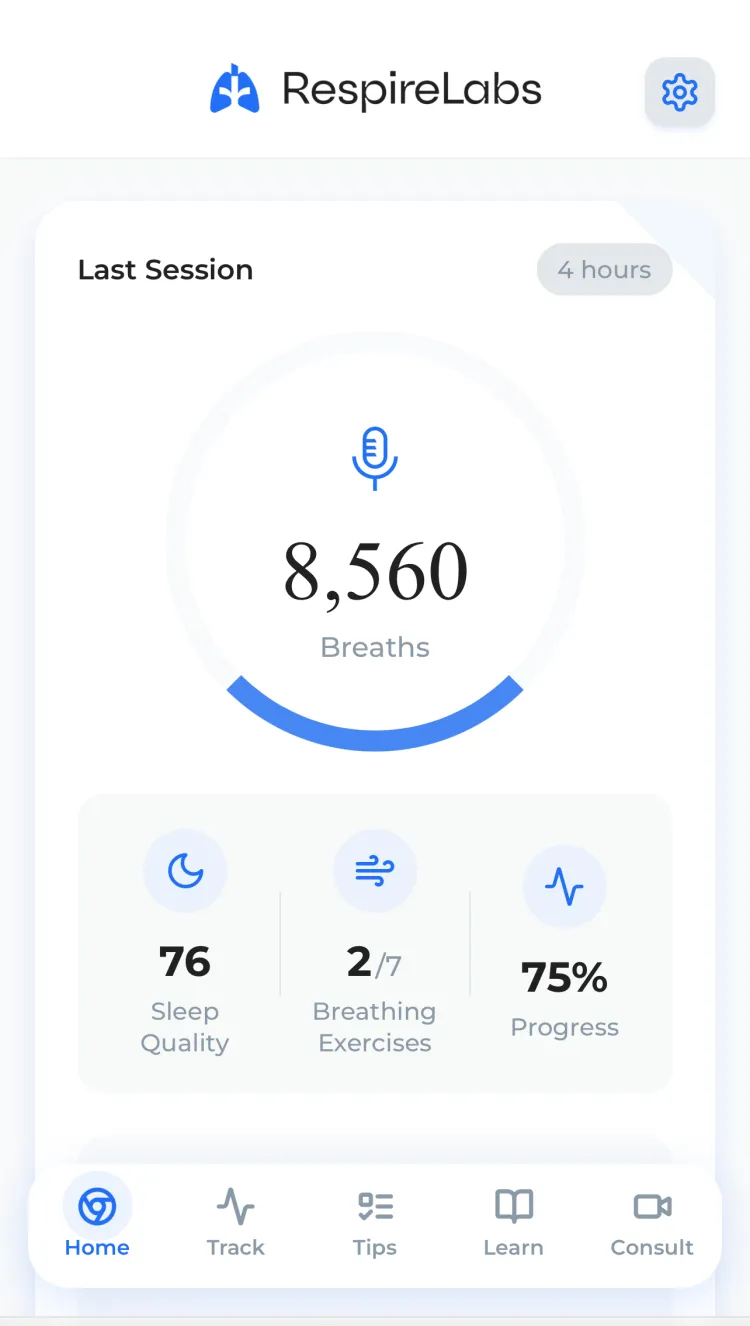
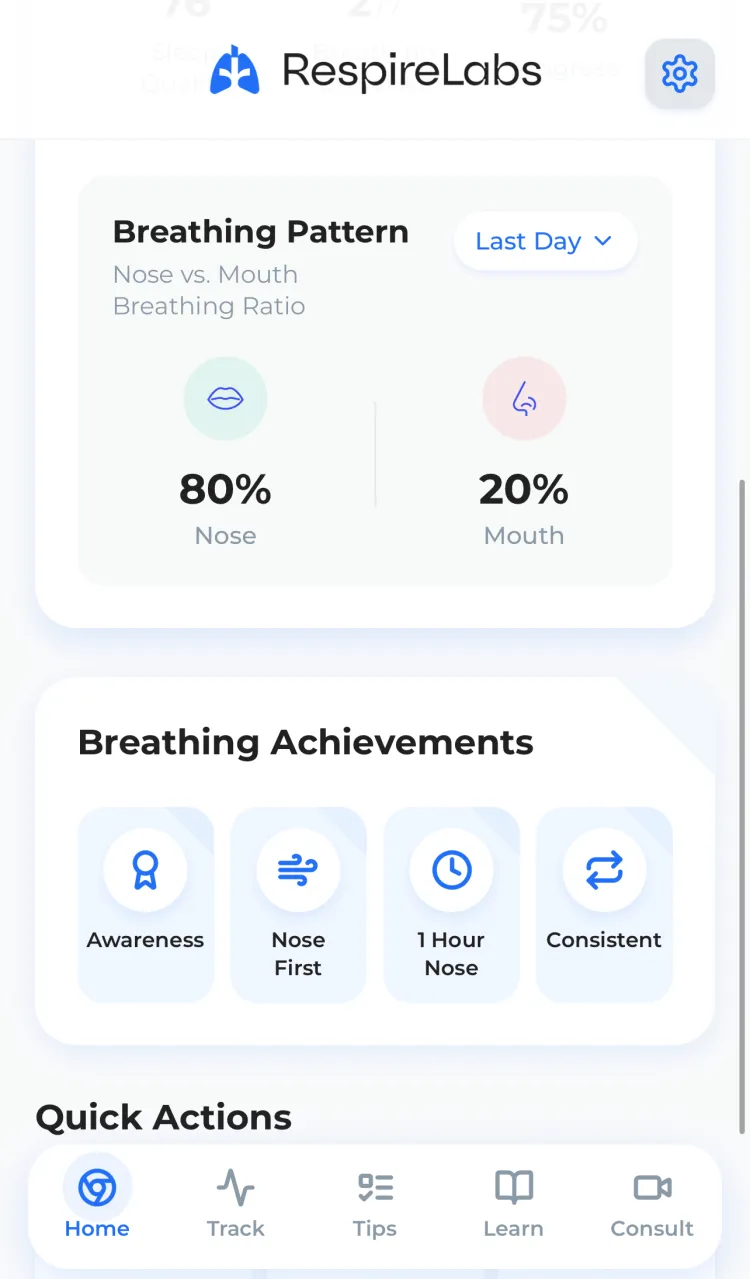
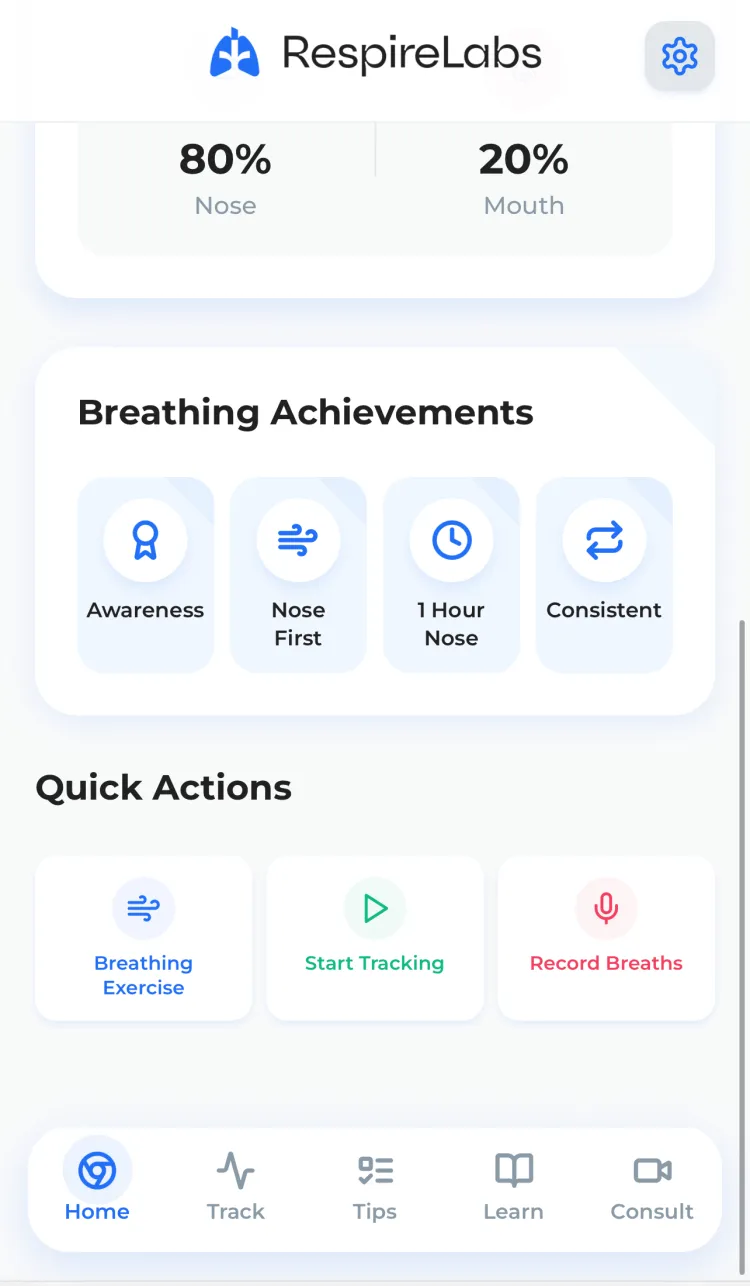
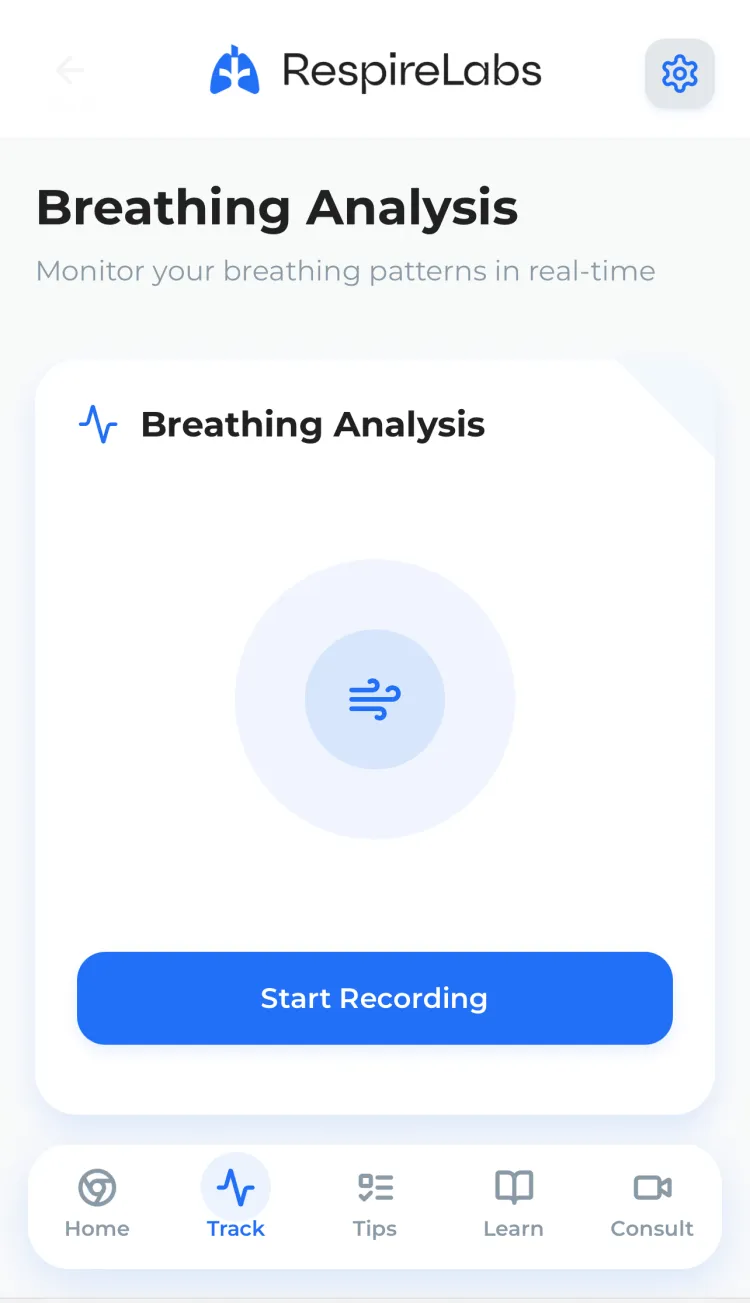
Meet RespireLabs.
Your breathing, tracked. Your habits, transformed.
Try this. Right now.
Close your mouth. Breathe only through your nose for half a minute. Just 5 breaths. Try to breathe so quietly that no one can hear it — not even you.
3 seconds in – 3 seconds out
When finished, try to keep on nose breathing. Whenever you realise you have your mouth open, come back to this exercise. This might seem small, but this is a foundation of building functional breathing habits.
Everything you need to breathe and sleep better.
Acoustic-AI, guided breathing exercises and direct access to expert teleconsultants who are ENT doctors, sleep coaches, breathing teachers and other professionals with deep expertise in sleep and respiratory health.
Breathing Detection
Real-time AI audio analysis detects mouth breathing using your phone's microphone.

Sleep Tracking
Track nose vs. mouth breathing ratio overnight.

Guided Exercises
Evidence-based breathing exercises tailored for you.
Achievements
Stay motivated with gamification and streaks.

Teleconsultation
Connect with breathing specialists.
Be a Founding Member.
Exclusive perks for early waitlist members.
Test Smart Tape
Selected 50 users will receive a sample kit. The only opportunity to test the early prototype.
Founding Member Badge
Special lifetime discounts on subscriptions and future smart wearables.
Priority Access
Be the first: a) to get the app. b) to claim a spot at our breathing retreat. c) to get the Smart Tape.
Founder Chat
Once we have the first 100 users on board, we will invite you to a private WhatsApp group chat. Your direct line to the RespireLabs team.
Shape the Roadmap
Express your needs and we will implement them. Vote on features and shape the future of RespireLabs products — they are for you.
Three steps to better breathing.
Download the app
Available on iOS and Android. Set up in under a minute.


Start a session
Our AI detects mouth breathing in real time using your phone's microphone.
Build the habit
Track progress, complete exercises, earn achievements. Watch your breathing improve.

"Your breathing, your data, your control."
Goes further with Smart Tape.
Pair the app with our Smart Mouth Tape for overnight tracking with clinical-grade sensors.
Quick answers.
Is RespireLabs a medical device?
Which phones does it work with?
When does it launch?
Is my data safe?
Who are Founding Members?
Are Founding Member spots limited?
What is the price?
References
- Fitzpatrick MF, McLean H, Urton AM, Tan A, O'Donnell D, Driver HS. Effect of nasal or oral breathing route on upper airway resistance during sleep. JAMA Otolaryngol Head Neck Surg. 2024. doi:10.1001/jamaoto.2024.3085
- Young T, Finn L, Kim H. Nasal obstruction as a risk factor for sleep-disordered breathing. JAMA Intern Med. 1997;157(21):2461–2466. doi:10.1001/archinte.1997.00440420077008
- American Academy of Sleep Medicine. National indicator report: importance of prompt sleep apnea diagnosis & treatment. AASM. 2023. aasm.org
- Lofaso F, Coste A, d'Ortho MP, Zerah-Lancner F, Delclaux C, Goldenberg F, Harf A. Nasal obstruction as a risk factor for sleep apnoea syndrome. Otolaryngol Head Neck Surg. 2007;137(4):569–574. doi:10.1016/j.otohns.2007.04.016
